Root resorption is a condition where the body gradually breaks down and absorbs parts of a tooth’s root. While this may sound unusual, it is a recognized dental issue that can affect both adults and children. In many cases, it progresses quietly and may not be noticed until it becomes more advanced. That is why Root Resorption Repair is often discussed in terms of early detection, protecting tooth stability, and planning for teeth preserving outcomes whenever possible.
Understanding the basics of how root resorption develops can help patients make sense of the diagnosis, recognize possible warning signs, and understand why careful evaluation of tooth root structure is essential.
What Root Resorption Means and Why It Matters
What happens inside the tooth
A healthy tooth root supports the crown and anchors the tooth within the jaw. Root resorption occurs when cells begin to dissolve and absorb the root surface or internal tooth structures. Over time, this can weaken the tooth’s foundation. Since the root is below the gumline, many of the early changes are not visible without professional assessment.
In discussions about Root Resorption Repair, the priority is often protecting function and preventing further loss of tooth root structure. The long term goal is usually to maintain stability, avoid complications, and support teeth preserving decisions when appropriate.
Internal vs external root resorption
Root resorption is commonly described in two categories:
Internal resorption begins from inside the tooth, often affecting the inner dentin and expanding outward.
External resorption begins on the outer root surface, gradually affecting the tooth from the outside in.
Both forms can lead to structural weakening, but they differ in appearance on imaging and in how they typically progress. A clear diagnosis helps identify which pattern is present and what risks it may pose to the tooth.
Tooth Root Structure Explained (and How Resorption Affects It)
The anatomy of a healthy tooth root
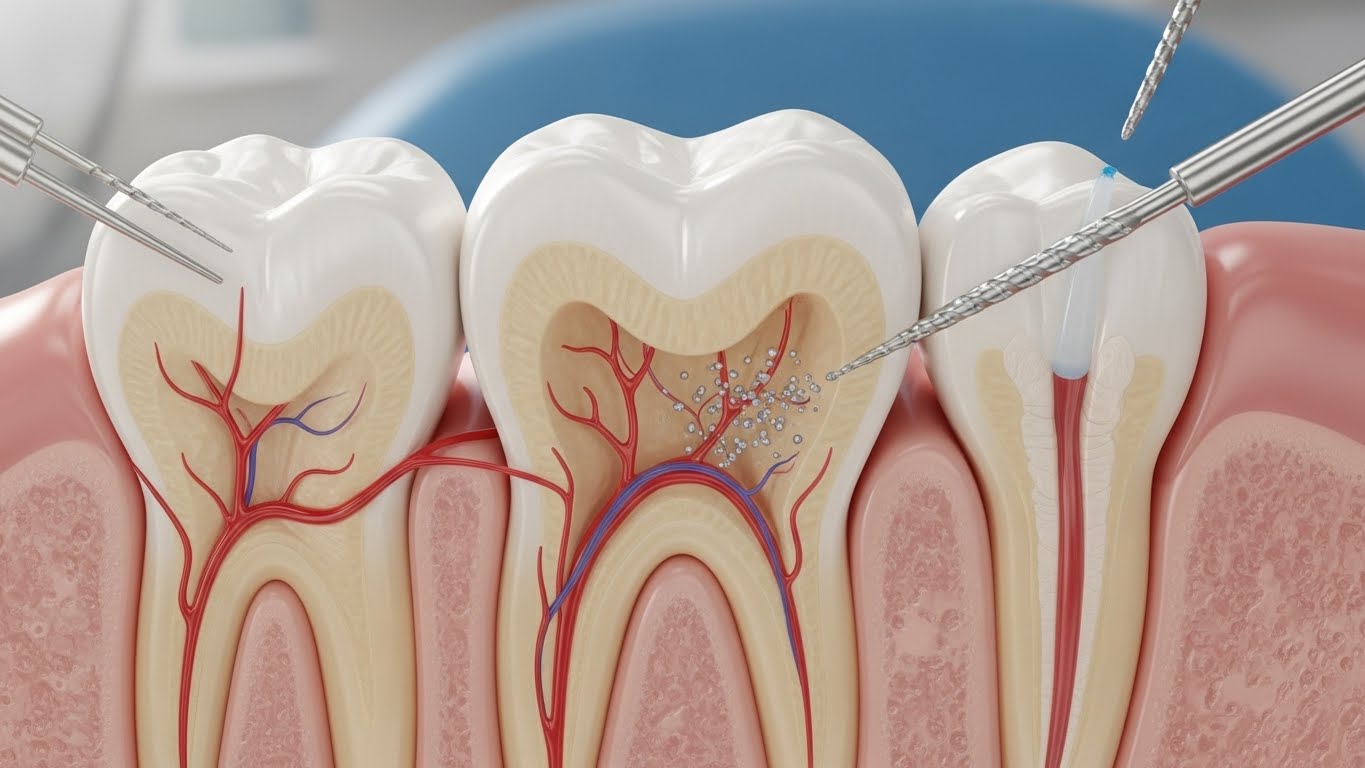
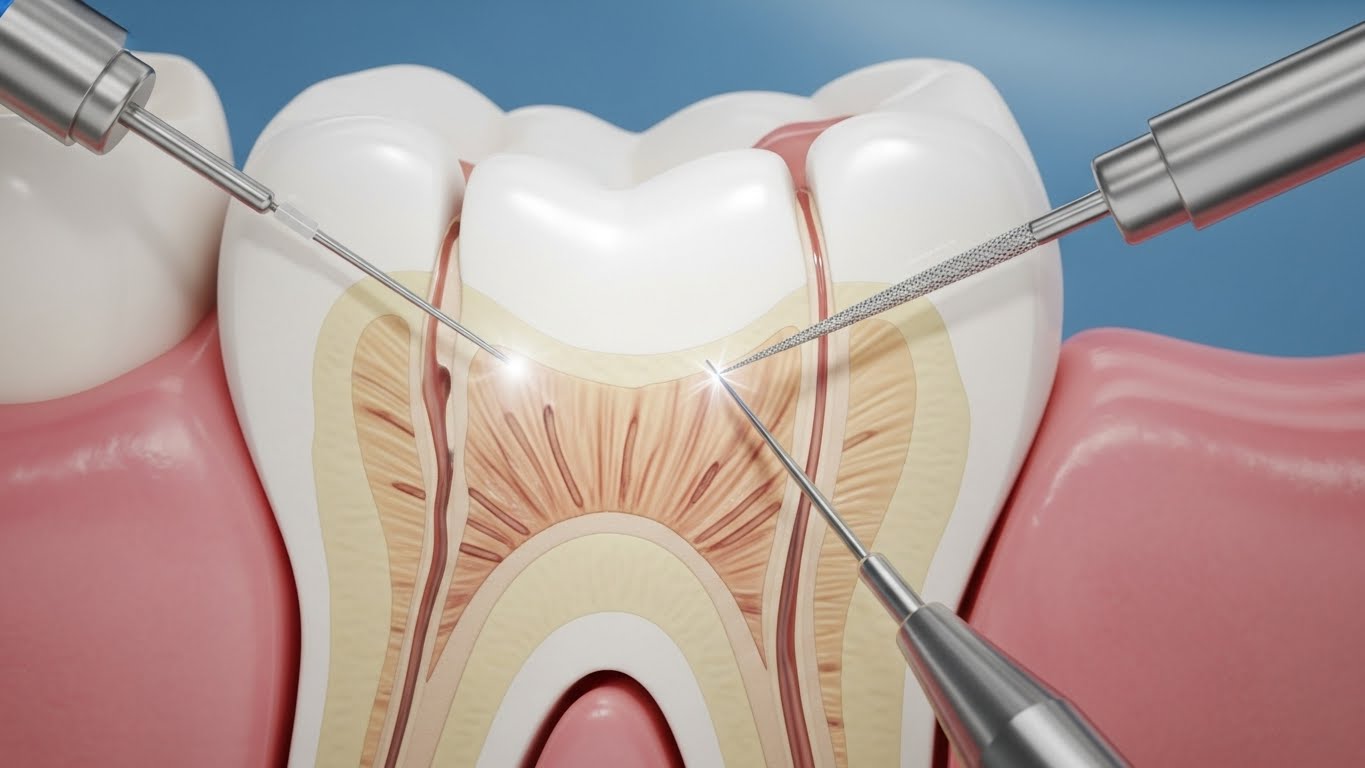
Tooth root structure is more complex than it appears. The root is made of layers of tissue that work together to support chewing, biting, and stability. It includes dentin (a strong inner structure), cementum (the outer covering), and the pulp space (where nerves and blood vessels are located). Surrounding the root is the periodontal ligament and bone, which help hold the tooth in place.
When resorption begins, some of these layers can be disrupted. As the root shape changes, the tooth may become less stable, particularly if the resorption affects key supporting areas.
Why root damage is hard to detect early
Because root resorption happens under the gumline, it often goes unnoticed. Many people do not feel symptoms in the early stages, and changes may only be visible on dental imaging. This is why regular evaluation is often the only reliable way to identify early changes in tooth root structure before they become severe.
Common Causes and Risk Factors of Root Resorption
Dental trauma and prior injuries
A previous injury such as an impact, fall, or accident can influence how tissues around the tooth respond over time. Even if the tooth felt fine after the event, cellular changes may develop later. Trauma is one of the most commonly discussed contributors to external root resorption.
Orthodontic history and pressure changes
In some cases, a history of orthodontic movement is discussed as a possible factor. Teeth shift through the bone with controlled pressure, and the body’s response to that pressure varies by individual. For some patients, that response may include changes to the root surface.
Inflammation and root infection
A root infection can influence surrounding tissues, especially when inflammation develops around the root. Infection-related processes may be associated with tissue breakdown, which is why the relationship between root infection and root resorption is often reviewed carefully during diagnosis.
Other contributing factors
Root resorption can also appear without an obvious cause. Individual biology, immune response, prior dental history, or tooth development patterns may play a role. Since root resorption is not always linked to a single clear trigger, evaluation typically considers the full picture.
Root Resorption Symptoms and Warning Signs
Possible symptoms people notice
Some patients experience symptoms, while others do not. Potential warning signs may include:
- Tooth sensitivity that feels new or unusual
- Discomfort when biting or chewing
- Swelling or tenderness around the gums
- Changes in tooth color
- A feeling that the tooth sits differently when biting
These symptoms can overlap with other dental issues, so they do not confirm root resorption on their own. However, they can prompt further evaluation.
Why symptoms are not always present
Root resorption can progress without pain, especially in early stages. If nerves are not affected and inflammation is limited, a patient may feel nothing at all. This silent progression is one reason why Root Resorption Repair discussions often emphasize diagnosis and monitoring rather than relying on symptoms.
How Root Resorption Is Diagnosed
Dental examination and clinical evaluation
Diagnosis typically begins with an evaluation of the tooth, surrounding gums, and overall oral health. A clinician may review symptoms, dental history, and any previous injury or orthodontic background. They may also check the tooth’s stability and look for signs of inflammation.
Imaging and what it can reveal
Dental imaging is essential for identifying changes below the surface. X rays can show root shape changes, loss of structure, or areas where the root surface appears irregular. In some situations, 3D imaging can provide additional clarity, particularly when evaluating the location and extent of changes in tooth root structure.
Tracking changes over time
Root resorption is sometimes assessed by comparing images taken at different times. This can help determine whether the condition appears stable or progressing, and it can clarify the level of risk for the tooth.
Root Resorption Repair and Teeth Preserving Goals
What “repair” means in dentistry
Root Resorption Repair is often used as a broad term describing efforts to protect the tooth’s role in function and preserve structural integrity. It may involve stabilizing a tooth, addressing underlying causes, and preventing ongoing damage. The approach and terminology can vary depending on the type and severity of resorption.
Teeth preserving considerations
Teeth preserving decisions often depend on factors such as:
- How much root structure is affected
- Whether the resorption is internal or external
- The tooth’s location and importance in bite function
- The health of surrounding bone and gum tissue
- Whether there are signs of root infection or inflammation
In many cases, the goal is to maintain tooth stability, avoid avoidable tooth loss, and protect surrounding structures.
When tooth extraction becomes part of the conversation
In advanced situations, tooth extraction may be discussed when tooth root structure is no longer sufficient to support function. This is not a reflection of failure, but rather a structural reality in some cases. The key point is that tooth extraction typically enters the conversation when the tooth’s long term stability becomes uncertain.
Complications and Why Timing Matters
Structural weakening and fracture risk
As resorption progresses, the tooth may become weaker. A tooth with reduced root support may be more vulnerable to loosening or fracture, especially under normal biting pressure.
Bite changes and functional impact
If a tooth becomes unstable, it can influence the bite and how pressure is distributed across other teeth. Over time, this may affect chewing comfort and overall oral function. This is why early recognition and assessment are emphasized in Root Resorption Repair discussions.
Conclusion
Root resorption is a serious condition because it affects the foundation of the tooth. Since it often progresses quietly, understanding warning signs, reviewing risk factors such as trauma or root infection, and evaluating tooth root structure through imaging are essential steps in managing the condition. Root Resorption Repair focuses on preserving stability, supporting teeth preserving outcomes when possible, and understanding when tooth extraction may become part of long term planning. With the right evaluation and clear diagnosis, patients can better understand their situation and make informed decisions with the help of their dental provider.
FAQ
- What is Root Resorption Repair in dentistry?
Root Resorption Repair refers to clinical efforts focused on protecting tooth stability when root structure is being absorbed or broken down. The term is often used to describe preserving function and preventing further damage to tooth root structure. - How does root resorption damage tooth root structure?
Root resorption changes the root’s shape and strength by gradually dissolving areas of dentin, cementum, or internal tooth structure. This can reduce the tooth’s ability to stay stable under normal bite pressure. - Can root resorption happen without symptoms?
Yes. Root resorption often develops silently, especially in early stages. Many cases are discovered through dental imaging rather than symptoms. - What is the difference between internal and external root resorption?
Internal root resorption begins inside the tooth and expands outward, while external root resorption begins on the outer surface of the root and progresses inward. The distinction is important because each type may present differently on imaging. - Can a root infection increase the risk of root resorption?
A root infection can contribute to inflammation around the tooth, and inflammatory processes may be associated with changes to tooth root structure. A dental evaluation helps clarify whether infection is part of the overall picture. - How is root resorption typically detected on dental imaging?
Root resorption is often identified when images show changes in root shape, thinning areas, or irregular patterns along the root surface or within the tooth. In some cases, 3D imaging may offer more detail. - Why do dentists focus on teeth preserving in root resorption cases?
Teeth preserving is often a priority because maintaining the natural tooth can support bite balance, chewing function, and jaw health. Decisions depend on how much tooth root structure remains and whether the tooth appears stable. - When does tooth extraction become a consideration with root resorption?
Tooth extraction may be discussed when the remaining root structure cannot support the tooth reliably, especially if the resorption is advanced or the tooth becomes unstable. - Does root resorption always mean a tooth will be lost?
Not always. Some cases progress slowly or remain stable, depending on the type and extent. Imaging and evaluation help clarify the severity and likely risks.
- How does root resorption affect long term oral function?If root resorption weakens a tooth significantly, it may affect chewing comfort and bite stability. In some cases, changes in one tooth can influence how pressure is distributed across surrounding teeth.